Vitamin D: Why Testing and Treatment Matter
Vitamin D often flies under the radar when we talk about essential nutrients, but this sunshine vitamin plays a vital role in keeping your body...
Consultation Required
Walk-in Friendly
Better results come with consistency. Our curated bundles pair treatments for enhanced benefits and better pricing each visit.
See Bundle PricingWellness builds over time. Our curated bundles pair complementary treatments for lasting results and preferred pricing.
See Bundle PricingThis is still a hot topic and the center of many social media debates as to where to actually get testing, what test you should ask for, and the accuracy of the test.
While many people have their opinions, it’s always best to look at the evidence and science first prior to making a decision yourself.
Keep reading to take a deeper dive into the different types of testing currently available for COVID-19, today, and which tests give specific infection information and data.
See here for updates on Long Covid; prevention, countering the effects, and getting rid of symptoms like COVID-19.
There are two main categories of tests for assessing the presence or history of COVID-19:
Diagnostic Testing: To test whether you actually have the virus
Antibody Testing: To test whether you could have come in contact with the virus or have been infected in the past from the virus.
There has been a lot of news surrounding the use of antibody tests for COVID-19 as well as confusion about what the tests do.
Most people want to know which test they should ask for upon arriving at the clinic (with symptoms or not) and what the accuracy of the testing actually is.
In the most basic terms, antibody tests are used to determine if you have had a past COVID-19 infection, while PCR (or molecular based) tests are used to determine if you are currently infected.
There are several variations for each of these types of testing that we will dive into a bit further below.
 There are a few different types of viral diagnostic testing available to the public currently.
There are a few different types of viral diagnostic testing available to the public currently.
Molecular testing informs patients, physicians, or researchers of the presence of the pathogen, either by identifying its genetic material or identifying unique markers of the pathogen itself.
The test uses the exact viral ribonucleic acid (RNA) for SARS-CoV-2 (COVID-19) which remains in the body only while the virus is still replicating.
This type of testing usually requires samples from the patient that are likely to contain virus, such as nasopharyngeal swabs or sputum samples.
For diseases specific to the respiratory tract, such as COVID-19, nasopharyngeal swabs have been considered to be the most reliable, as they sample an area of the respiratory tract where the virus appears to first infect an individual.
For more in-depth knowledge around how molecular testing works, click HERE to learn and see many of the pro’s and con’s of different methods.
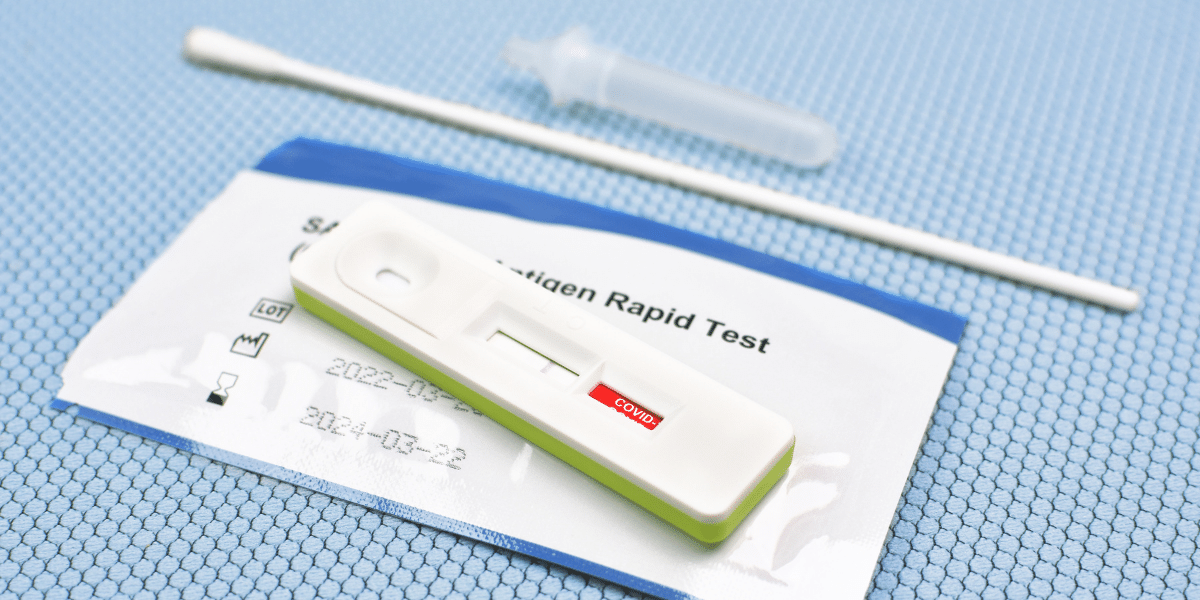
Antigen tests are another type of diagnostic test (to test if you have the active virus).
While antigen tests are newer to the market and can provide faster results, antigen tests have a higher chance of missing an active infection.
For example, if an antigen test shows a negative result (indicating that you do not have an active coronavirus infection) your health care provider may order a molecular test to confirm the result.
This is similar to how a pregnancy test works. If you see the positive result on the at home test, usually follow up blood work is warranted to confirm the results.
The main difference that most consumers are worried about is ease of testing and accuracy.
While PCR tests can be incredibly accurate, obtaining the samples and analyzing the results can take time.
On the flip side, one of the main advantages of an antigen test is the speed of the test, which can provide results in minutes.
But (and this is the most important factor), antigen tests may not detect all active infections, as they do not work the same way as a PCR test.
Even though antigen tests are very specific for the SARS-COV-2 virus, they are not as sensitive as molecular PCR tests.
 Antibody testing is not supposed to be used to "diagnose" an active infection from the virus, but can be extremely useful to see if you have been in contact with or have been infected from the virus in the past.
Antibody testing is not supposed to be used to "diagnose" an active infection from the virus, but can be extremely useful to see if you have been in contact with or have been infected from the virus in the past.
Whenever the immune system is confronted with a disease-causing organism like a virus, it produces defensive proteins called antibodies.
These antibodies are then stored for future use in the case that the organism comes back in contact with that exact virus.
The antibodies are matched specifically to that organism so that they can prevent a future infection down the road and are the main mechanism behind how vaccines work for specific diseases.
COVID-19 antibody tests are looking for the antibodies made in response to exposure to the SARS-CoV-2 virus.
There are two main types of antibodies, which are also called immunoglobulin (Ig), that the body can produce in response to a COVID-19 infection:
Antibody tests may provide quick results, but should not be used to diagnose an active infection. That is what the diagnostic/molecular based testing is for.
Antibody tests only detect antibodies the immune system develops in response to the virus, not the virus itself.
The key to remember is that it can take days to several weeks to develop enough antibodies to be detected on a test.
There are two main tests available for testing for COVID-19 antibodies:
Most people would prefer to pay less money and have quicker results for their testing.
And who could blame them?
But the issue is that per the research and current results, serum testing is much more reliable and accurate when it comes to testing for antibodies.
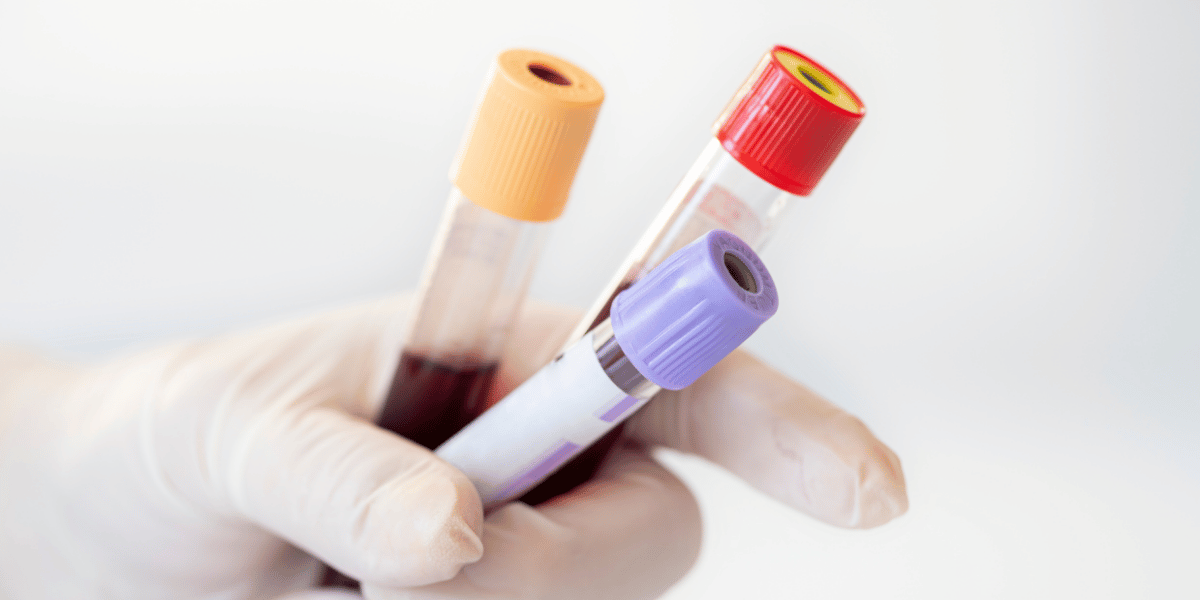
Similar to the at-home pregnancy test analogy above, drawing blood to test for antibodies requires a full sample to be taken from the patient, then the sample if spun down and placed on specific lab instrumentation in order to detect antibodies.
Just like the PCR testing is more accurate than the antigen testing for the actual viral infection, drawing a sample of blood is much more accurate than simply using a finger prick to detect antibodies for COVID-19.
While it is always great to know if you have had the virus or if you potentially have immunity to it, another great reason to test for Antibodies is that the U.S. Food and Drug Administration (FDA), in partnership with the American Red Cross, is encouraging people 17 and over who weigh more than 110 pounds to donate blood if they have a positive COVID-19 antibody test results.
Although more research is needed, they believe the transfusion of defensive antibodies may help severely ill people better fight and recover from a COVID-19 infection.
Click below to contact us and ask how we can help!
Disclaimer: The information provided in this blog regarding the potential benefits of micronutrients is for informational purposes only. While micronutrients may offer various health benefits, we do not make any claims or guarantees regarding the effectiveness of these nutrients for specific health conditions. Micronutrients should not be considered a treatment for any illness or medical condition. Our goal is to offer supportive therapy to the body, and we recommend consulting with a qualified healthcare professional before making any changes to your diet or supplement routine.
 Drip IV is a leader in the delivery of intravenous micronutrient therapies servicing Lafayette, Louisiana and the surrounding areas. As a drip infusion bar, we provide GLP-1 medications for weight loss, NAD+, and IV nutrition therapies for Energy, Hydration, Immunity, Performance & Recovery, which may benefit COVID-19 and Long COVID symptoms and recovery.
Drip IV is a leader in the delivery of intravenous micronutrient therapies servicing Lafayette, Louisiana and the surrounding areas. As a drip infusion bar, we provide GLP-1 medications for weight loss, NAD+, and IV nutrition therapies for Energy, Hydration, Immunity, Performance & Recovery, which may benefit COVID-19 and Long COVID symptoms and recovery.
Lafayette: 4906 Ambassador Caffery Pkwy, Bldg. B, Lafayette, LA 70508

Vitamin D often flies under the radar when we talk about essential nutrients, but this sunshine vitamin plays a vital role in keeping your body...
Micronutrients play a crucial role in our overall health, yet their importance is often overlooked. From boosting immune function to supporting ...

With all the panic around COVID-19 and most of the population directing their attention towards social distancing, washing their hands, and wearing...